Health-care productivity
Health-care productivity measures health-care outcomes against resources (usually money) employed. If the metric measured is against resorces spent directly on potentially relevant health-care, productivity can be estimated.
Strictly it is different from health productivity as a measure of health in a population such as life expectancy depends also upon a cultures prioritisation in fields as diverse as education, infrastructure and reduction in addressable social inequalities. Societies should generally be more interested in health productivity. The same incremental public health-care intervention such as safer water supply may result a significant impact on health productivity in a third world country, but not a first world country. On the other hand investing in primary-PCI will almost certainly make no useful impact on either health productivity or health-care productivity metrics for the whole population in a third world country but may well to do for a small segment of that countries population or for the whole population of a first world country.
Some of the most irreconcilable debates on health or health-care productivity can be objectively analysed as debates based on different value systems. For example a health-care productivity metric that utilised complication rates of therapeutic abortion is rather likely to be subjectively interpreted in some value systems. However all possible metrics come with differential value in different value systems. As illustrated in the examples below the confounders can be very marked.
Contents |
Issues
Gains in health-care productivity have in developed nations lagged considerably behind many other sectors of the economy. Roemer’s Law is only part of the reason for this. Indeed health care can become more effective if individualised while some of largest gains in productivity result from investments in a single product capable of mass market economies of scale. This actually implies that societies will have increasing issues in resourcing health care. Major causes are believed to be the need to individualise health-care interventions and the reliance on health-care workers to deliver ever more complex interventions not open to automation. Regulation can often lower productivity, increasing costs, but so can stricter application of basic infection control procedures or use of technology that has a cost inflation rate far above other sectors of the economy. How do you compare gains in public health with gains in cancer cure rate, with the later having a markedly lower productivity per monetary unit spent relative to any basic health care metric ?. The metrics chosen can show marked cultural variation based on different value approaches. Do you value most,avoidable mortality[1], under 75 mortality, maternal mortality, neonatal mortality, pain control, morbidity caused by metal illness, infectious disease, cancer or say neurodegenerative disease ?.
General Approach
- Clinical engagement and workforce incentives provide a means to drive motivation for improvement
- New ways of working provide a means to improve efficiency and reduce inputs
- Tackling variation through measurements in order to improve productivity metrics and improve the quality and outcomes from health care[2]
Secondary Care
See Improving NHS productivity:The secondary care doctor’s perspective Kings Fund
Examples
New Zealand
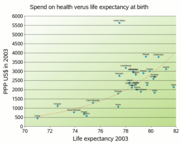
In terms of life expectancy at birth compared to amount of gross nation product spent on health care New Zealand appears to have health-care productivity only exceeded obviously by Spain and perhaps Japan figures (see Fig. 1). However even with-in New Zealand there are potentially addressable issues in terms of health and social policy that could increase this productivity. New Zealand has a less homogenous culture than either Japan and Spain. The major sub-cultures in New Zealand are Maori and non-maori polynesians. Compared to Europeans they have a higher rate of many illnesses, including infectious disease. This can be shown to be associated with ethnic and social inequalities, and has been increasing particularly since 1994. The 1990's were a period of changed economic policy with raising income inequality and it can be postulated that health-care associated interventions that have occurred in New Zealand have been unable to compensate for economic or social policy that has a greater influence on what appears to be superficially a health-care metric[3].
USA
The unsustainable, almost exponential increase in per capita health expenditure from in the USA health economy[4] has not been associated with gains in any health associated metric that other societies have not been able to deliver, so resulting for them in greater health-care productivity. This may reflect fee for service, rather than fee for bundle of care approaches and excessive administration due to healthcare system design.
UK
A national audit office report identified decreasing hospital productivity of 1.4% a year. However analysis of this report more objectively suggests that issues of the metrics chosen and interpretation for political gain could have created a myth[5]. It may be very easy to create and sustain such myths when due to external factors such as the European Working Time directive there has been a large expansion in the clinical workforce, absorbing much of the increased funding, which will certainly impact in areas such as elective surgery where capacity for innovation may be limited. In some areas of health care that may be more important for population health such as care of ischaemic heart disease there have been marked health-care productivity gains. When analysis of the data suggests that a number of elective surgical measures contributed to the metric used far more than emergency and elective cardiology, the metric should be questioned[5].
External link
See International Health Care Systems — Selected Measures NEJM Interactive graphic WARNING Flash content[6]
References
- ↑ Castelli A, Nizalova O. Avoidable mortality: what it means and how it is measured. Centre for Health Economics, University of York; CHE Research Paper 63.
- ↑ [Charlton R, Imison C, Curzon J. How to get the best outcomes when measuring productivity. Health Service Journal 12 July]
- ↑ Baker MG, Barnard LT, Kvalsvig A, Verrall A, Zhang J, Keall M, Wilson N, Wall T, Howden-Chapman P. Increasing incidence of serious infectious diseases and inequalities in New Zealand: a national epidemiological study. Lancet. Feb 17.(Link to article – subscription may be required.)
- ↑ Fuchs VR. Major trends in the U.S. health economy since 1950. The New England journal of medicine. Mar 15; 366(11):973-7.(Link to article – subscription may be required.)
- ↑ a b Decreasing NHS productivity: urban myth. Lancet. Feb 18; 379(9816):590.(Link to article – subscription may be required.)
- ↑ International health care systems--selected measures. The New England journal of medicine. Jan 1; 372(1):e1.(Link to article – subscription may be required.)